DBT for Depression: How It Works and Helps You Feel Better
Depression can make even simple daily tasks feel overwhelming, and traditional talk therapy doesn't always provide the practical tools you need to manage difficult emotions. That's where DBT for depression comes in, a structured, skills-based approach that goes beyond conversation to give you concrete strategies for changing how you think, feel, and respond to life's challenges.
Dialectical Behavior Therapy was originally developed for borderline personality disorder, but research now shows it's highly effective for treating depression too. The therapy combines acceptance techniques with behavioral change strategies, helping you build emotional resilience while learning to tolerate distress in healthier ways.
At New Path Counseling, our therapists in Gretna and Omaha use evidence-based approaches like DBT to help clients of all ages work through depression. Whether you're considering therapy for the first time or looking for a different approach than what you've tried before, understanding how DBT works can help you decide if it's the right fit. This guide breaks down the core skills, explains how treatment typically unfolds, and shows you what real progress can look like.
What DBT is and how it differs from CBT
Dialectical Behavior Therapy is a structured treatment approach that teaches you specific skills for managing emotions, tolerating distress, and improving relationships. The word "dialectical" refers to balancing two seemingly opposite ideas: accepting yourself as you are while also working to change unhelpful patterns. This dual focus sets DBT apart from many other therapy models, making it particularly useful when you're stuck between wanting things to be different and feeling unable to change them.
The core principles of DBT
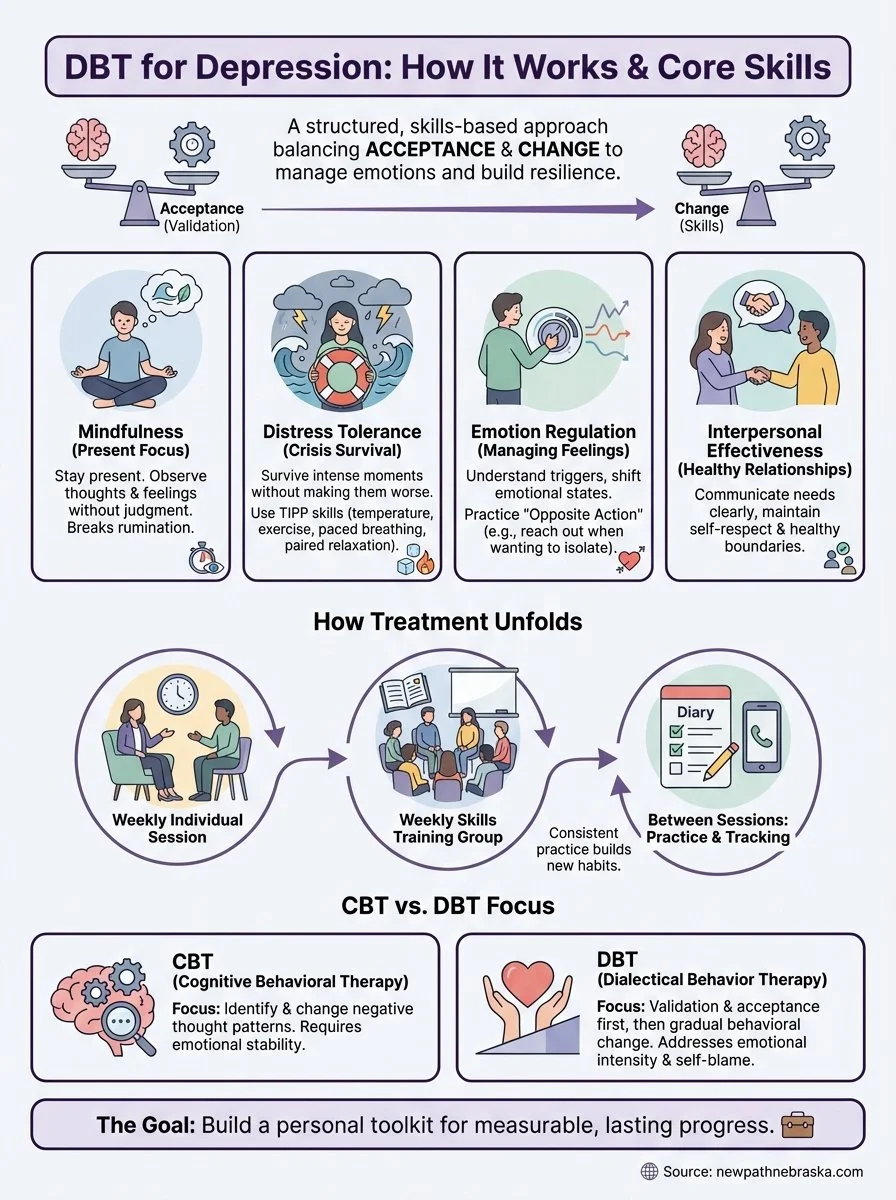
DBT organizes treatment around four main skill areas that you learn through weekly individual therapy sessions and group skills training. Mindfulness helps you stay present instead of ruminating on the past or worrying about the future. Distress tolerance gives you practical strategies for surviving crises without making things worse through impulsive actions. Emotion regulation teaches you to identify, understand, and shift intense feelings before they overwhelm you. Interpersonal effectiveness focuses on communicating your needs clearly while maintaining self-respect and healthy relationships.
Your therapist typically assigns homework between sessions where you practice these skills in real situations and track your progress using diary cards. This structured approach means you're actively building new habits rather than just talking about problems. The skills compound over time, giving you a toolkit you can use long after therapy ends.
DBT requires active participation and consistent practice between sessions, which is why it works best for people ready to commit to the process.
How CBT and DBT approach depression differently
Cognitive Behavioral Therapy focuses primarily on identifying and changing negative thought patterns that fuel your depression. You work with your therapist to challenge distorted thinking, test out beliefs, and gradually change behaviors that keep you stuck. CBT is highly effective, but it assumes you have enough emotional stability to examine your thoughts rationally and complete assignments between sessions.
DBT for depression adds acceptance-based strategies that CBT doesn't emphasize as strongly. When you're in the middle of a depressive episode, trying to "think differently" can feel impossible because your emotions are too intense. DBT acknowledges this reality by first teaching you validation and acceptance skills that help you tolerate difficult emotions without judgment. You learn that feeling depressed doesn't mean you're broken or doing something wrong, it's a signal that deserves compassionate attention.
Another key difference is how each approach handles behavior change. CBT often asks you to push through avoidance by doing activities even when you don't feel like it, which can backfire if you're not emotionally ready. DBT uses a more gradual approach that balances pushing yourself with self-compassion. You might start with small steps like getting out of bed for five minutes rather than forcing yourself into a full day of activities before you have the emotional skills to sustain it.
The group component in DBT also differs from traditional CBT. While some CBT programs include group sessions, DBT requires weekly skills training in a group setting where you practice with others facing similar challenges. This creates accountability and lets you learn from others' experiences in real time.
Why DBT can help with depression
Depression often creates a cycle where negative emotions trigger self-criticism, which deepens the depression and makes it harder to take positive action. You might judge yourself for feeling bad, then feel worse about judging yourself, creating a downward spiral that traditional talk therapy doesn't always interrupt. DBT for depression breaks this pattern by teaching you to accept difficult emotions while simultaneously building skills to manage them more effectively.
DBT addresses the emotional intensity of depression
Depression isn't just sadness, it involves overwhelming feelings that can shift rapidly throughout the day. You might wake up feeling numb, experience intense hopelessness by afternoon, then feel irritable or anxious by evening. These emotional swings exhaust your mental energy and make it difficult to maintain consistent self-care habits or complete daily responsibilities.
DBT specifically targets this emotional dysregulation by teaching you concrete techniques for recognizing when emotions start escalating. You learn to identify physical sensations that signal emotional shifts, like tension in your chest or changes in your breathing pattern. The distress tolerance skills give you immediate strategies for getting through intense moments without making impulsive decisions you'll regret later, such as isolating yourself or engaging in self-destructive behaviors.
DBT gives you tools to ride out emotional waves instead of getting pulled under by them.
The validation approach reduces depression's self-blame
Depression convinces you that feeling this way is your fault, that you're weak or broken for struggling when others seem fine. This self-judgment intensifies your symptoms and prevents you from seeking help or practicing self-compassion. Traditional therapy sometimes accidentally reinforces this pattern by immediately jumping to problem-solving before acknowledging how hard things actually are for you.
DBT takes a different approach by first validating your experience as understandable given your circumstances and biology. Your therapist helps you recognize that depression is a real condition affecting your brain chemistry and thought patterns, not a character flaw. This validation doesn't mean accepting defeat, it means reducing the extra suffering you create by beating yourself up for having depression in the first place. When you stop wasting energy on self-criticism, you free up mental resources for actual healing and skill-building.
How DBT for depression works in real life
DBT for depression follows a structured weekly format that combines individual therapy sessions with group skills training. You typically meet with your therapist one-on-one for 50 to 60 minutes each week to work through personal challenges and review how you're applying skills in your daily life. Separately, you attend a weekly group session lasting about two hours where you learn new DBT skills alongside others who are also working to manage difficult emotions. Between sessions, you complete homework assignments and fill out diary cards that track your mood, urges, and skill use.
What your first weeks of treatment look like
Your therapist starts by conducting athorough assessment of your depression symptoms, life circumstances, and treatment goals during the initial sessions. You work together to identify specific behaviors you want to change, such as social isolation, sleep problems, or patterns of self-criticism that worsen your mood. This assessment phase helps create a personalized treatment plan that targets your most pressing challenges while building a foundation of basic DBT skills.
During these early weeks, you begin learning mindfulness techniques that form the core of all other DBT skills. Your therapist teaches you simple practices like observing your thoughts without judgment or describing emotions without getting swept away by them. These skills feel awkward at first because depression makes it hard to focus, but consistent practice helps you notice patterns in your thinking and emotional responses that you couldn't see before.
How the skills build on each other over time
As you progress through treatment, you add new skill modules while continuing to practice earlier ones in increasingly complex situations. You might start by using distress tolerance techniques to survive difficult moments without making things worse, then layer in emotion regulation skills that help you understand what triggers your depressive episodes. The interpersonal effectiveness skills come later once you have enough emotional stability to handle relationship challenges without becoming overwhelmed.
Real change happens through repeated practice in situations that matter to you, not just during therapy sessions.
Most people noticemeasurable improvements within three to six months as the skills become more automatic and require less conscious effort. You develop a personal toolkit of strategies that work specifically for your depression patterns, making you less dependent on your therapist over time.
Key DBT skills that target depression symptoms
DBT for depression teaches you four main skill categories that directly address the emotional, cognitive, and behavioral symptoms keeping you stuck. Each skill set gives you practical techniques you can use immediately when depression makes everyday functioning difficult.Your therapist typically introduces these skills gradually, starting with mindfulness as the foundation and building toward more complex interpersonal strategies as your emotional stability improves.
Mindfulness stops rumination before it spirals
Depression thrives on repetitive negative thinking about past failures or future catastrophes. Mindfulness skills train you to observe these thoughts without getting caught in them, creating distance between you and the depressive narrative running through your mind. You practice simple techniques like focusing on your breath for 30 seconds or describing what you see around you in objective terms, which interrupts the rumination cycle before it takes over your entire day.
The "observe and describe" skill proves particularly useful when you notice yourself spiraling into self-criticism. Instead of believing every negative thought, you learn to label it as just a thought rather than absolute truth. This shift doesn't make the thoughts disappear immediately, but it reduces their power to control your mood and actions.
Emotion regulation targets the biology of depression
These skills help you understand what triggers your depressive episodes and develop strategies for shifting your emotional state before it becomes overwhelming. You learn to identify the physical sensations, thoughts, and urges that accompany depression, then apply specific techniques to regulate your nervous system. The "opposite action" skill is especially effective when depression tells you to isolate yourself or stay in bed all day.
Opposite action means doing the opposite of what your depressive urges tell you, like reaching out to a friend when you feel like withdrawing completely.
Building positive experiences through pleasant activities scheduling also falls under emotion regulation. You deliberately plan small, manageable activities that align with your values, gradually rebuilding your capacity for enjoyment even when motivation feels absent.
Distress tolerance prevents destructive coping
When depression feels unbearable, you need crisis survival skills that get you through intense moments without making things worse. Techniques like the TIPP skill (temperature, intense exercise, paced breathing, paired muscle relaxation) help you calm your nervous system quickly during acute distress. These aren't long-term solutions, but they prevent impulsive decisions or harmful behaviors when your depression peaks.
How to practice DBT skills between sessions
DBT for depression requires consistent practice outside of therapy sessions to create lasting change. Your therapist gives you homework assignments and diary cards to complete each week, but the real progress happens when you apply skills during actual emotional challenges rather than just reviewing them during calm moments. Most people struggle with this at first because depression drains motivation, but building a simple practice routine makes skill use feel less overwhelming over time.
Create a daily skills tracking system
Setting up a structured tracking method helps you remember which skills to practice and shows you patterns in what works for your specific depression symptoms. You can use a simple notebook, your phone's notes app, or the diary cards your therapist provides to record when you used a skill, what situation triggered the need, and how effective it was. This daily logging takes less than five minutes but creates accountability and helps your therapist identify which techniques deserve more focus during sessions.
Your tracking system should capture three key pieces of information: the intensity of your emotion before using a skill (rated 1 to 10), which specific technique you applied, and how you felt afterward. This data reveals whether certain skills work better for particular triggers, like using opposite action for isolation urges versus TIPP skills for acute anxiety during a depressive episode.
Tracking your skill use turns abstract concepts into concrete evidence of progress, even when depression tells you nothing is helping.
Start small and build consistency
Trying to practice every DBT skill immediately sets you up for failure and reinforces the hopelessness depression creates. Instead, pick one or two techniques that address your most pressing problems and commit to using them in specific situations for a full week. You might decide to practice mindful breathing every morning before getting out of bed or use the STOP skill (Stop, Take a step back, Observe, Proceed mindfully) whenever you notice self-critical thoughts starting.
Building consistency matters more than perfection. You won't apply skills correctly every time, and some days your depression will be too intense for any technique to feel helpful. The goal is developing a habit of turning toward these tools instead of defaulting to avoidance or numbing behaviors when emotions spike.
Next steps
DBT for depression gives you concrete skills that address the emotional intensity, negative thinking patterns, and behavioral problems keeping you stuck. The structured approach combines acceptance of where you are right now with practical strategies for building the life you want, creating measurable progress over time instead of just talking about your problems week after week.
Starting therapy requires courage, especially when depression makes everything feel harder than it should. You don't need to have all the answers or feel completely ready before reaching out. The therapists atNew Path Counseling work with adults, teenagers, and children across Gretna and Omaha using evidence-based approaches like DBT to help you develop skills that create lasting change.
Taking the first step means recognizing that your current strategies aren't working well enough and deciding to try something different. Whether you choose in-person sessions or teletherapy, professional support gives you the guidance and accountability needed to make DBT skills part of your daily life.